My Mom’s Journey
This page is an archive of e-mails sent in the finally portion of my Mom’s amazing journey. These messages were initally sent to just my brothers, then to an expanding group of family and friends.The Stumble
I'm out visiting Mom and she is not doing well. Her PO2 is 67 resting, Resp is 60' Pulse is 130.We called her Doc and they want her to go to the ER at Swedish First Hill on Broadway in Seattle.
I'm going to drop her dogs off at our house and then meet them there. I'll update you as soon as I can.
In the hospital
So, I just got to the hospital. Fred just went back with Mom. Sounds like they took her back pretty quick.Kim says that she is on 4Lpm (possibly 6) of O2, her PO2 was 92. (It can rise and fall sharply based on exertion and other mysterious factors.
Sounds like they may be doing the standard work up; blood, urine, chest X-ray, EKG.
I had not mentioned earlier that her ankles are significantly swollen bilaterally.
We are in the ER and she has not been admitted.
Vitals
BP = 132/79Pulse = 116
O2= 98
Resp= 36
Intervention
Sounds like Mom received a steroid injection (Methylprednisone 125mg) and a Nebulizer treatment (unk) after the ER Doc did a phone consult with her regular doctor. She is stable at this time.Being Admitted
They are going to keep her in the Hospital. The Doc was just in and is going to give her Lasix to get any fluid out. Someone from the Polyclinic (her PCP) will be in to see her later.And it starts...
So, lots to cover, and I'm sure I will leave stuff out. Here goes;Mom was moved to the Intermediate Care floor. She's in room 749 in the East tower. A Hospatilst with the Polyclinic saw her and did an EXTENSIVE history and probing about her current condition, previous interventions and associated data points. He also got the skinny on her current meds, including the modifications Mom has been making to her dosages.
He feels that there are possibly some other components at play here, including possibly heart failure. They did an ultrasound for DVT and she has compressions on her lower legs. They will do an echo tomorrow to gauge her heart status, especially as compared to a similar study done in 2010.
She will be seen by at least two other Hospitalists and Pulmunologists tomorrow. This doc thought she would have 3 or 4 additional opinions by the time she is discharged.
He also had a preliminary discussion with her about advanced directives. Mom was not at the point where she could communicate her preferences, which means that they will revive her if she goes into arrest. But the doctor made it clear that he thought her current weak state would mean that she would probably spend the remaining days of her life in a care facility of some sort if that were to happen.
The good news is that we're getting the second opinion we all wanted. The bad news is that her health has deteriorated in the last year, if not four years, and I'm not sure how much she'll be able to recover.
As far as orders; the doc is going to continue the IV steroids, add an antibiotic to clear up anything in her lungs, write an as-needed order for Morphine, discussed a low dose anti-anxiety, continue the Lasix to relieve swelling in the ankles and the possible CHF associated symptoms. I know I'm missing stuff, but its been a long day.
Rob - They use Epic for their EMR. Let me know if you want me to see if you can get access.
Patrick Hennessy, our cousin, will be here tomorrow night for a planned visit on Saturday, and then heading out early on Sunday.
I will be at the hospital very early tomorrow, probably before 5am. Fred will be in around 8 and we should have our first doctor swing by around then.
The First Morning
Just wanted to offer a brief update. Mom has been awake since I arrived at 4:30 this morning and is in good spirits. Her stats are good (110/62, 111, 20, 92) and she is breathing and conversing fine.Her memory is not serving well, and we will discuss the same topic three times in a 90 minute span. I attribute this to meds, but I'm not sure we really know where her mental baseline is anymore. She is frequently under the impression that she should be leaving here today, and is continually asking for coffee which she can't have.
They have her on 40mg of steroids every 8 hours and are continuing the Lasix at unknown dosing. Her weight is down to 120, so I expect a nutritionist visit today. Her doc last night put her on a cardio diet, but the nurses think that will change today.
The nurses related that Mom had a seizure like episode last night. They checked on her and she was unconscious and unresponsive. They initially moved her back up in the bed, and her eyes opened, but she would not respond verbally. She did follow commands, such as raising her arms when directed. They think neurology may take a peek at her. I think this was probably just her being confused/disoriented.
On the schedule for today should be a echocardiogram. I'll let you know more once we start to see Doctors here.
I'm going to hang here until midday, and then go home to get some sleep. Fred will be here during the day, and I'll relieve him around dinner time until I head home when Patrick arrives.
The First Night
Sorry for the delay in catching everyone up. I was here from 4:30 this morning until just after noon, and then headed home for some errands and rest. I just got back and am getting caught up.Mom's stats look good, and she is generally improving. She finished her lunch, which may be the first complete meal she's had in a month. I believe she's also lost some weight, but don't have solid data on that yet. It sounds like they may be moving her off of this ward tomorrow.
Fabio is here now, and Patrick is due in several hours.
She had an echocardiogram by ultrasound this morning, and we have not heard the initial findings by the cardiologist yet. Apparently a Pulmonologist made rounds and visited with her, but it does not sound like there were any new topics or findings. She felt that the cardiac issues (fluid retention) were a bigger problem.
They are continuing with respiratory therapy, steroids, diuretics, antibiotics, etc.
We have not had a diagnosis of any cardiac issues, and are awaiting that.
Mom has been on 40mg of diuretic, but her output had not increased.
Mom remains unable to retain information about her health or care. She has heard us discussing several times today the unresponsive episode from last night, and each time is a surprise to her which seems to alarm her. I think discussions about her health and care in the room may be disconcerting to her. She will hear about something relating to her care or health state and become alarmed. We then have to relate the entire condition and resolution to her, but the next time she hears of the same issue, it is a complete surprise and we have to go through the whole exercise again. I think being disconnected is difficult for her, while talk of puppies, wine and family is quite pleasant.
I feel like I missed a good chunk of the activity today, so I'm catching you up on second news as I get it. Fred is included on this message and might be able to answer any questions you may have. I'll be here for a while and will update you with any developments.
We had a great interaction with the Hospitalist covering last night, and hope to see him again tonight…
Family Update
Good Morning!So here's the update from the hospital. I arrived around 6:50am or so and Mom was about 15 minutes into a Panic/Paranoid episode. (The nurses were attempting to call me when I arrived.) Her first words to me were "I'm panicking." I made some considerable effort to get her to accept the 0.5mg of Ativan (anti-anxiety) that she and the Doctor had agreed yesterday would be helpful if an episode occurred. She felt that the staff were not interested in helping her and that she did not trust them. She wanted to contact Steve Shambaugh (an old friend) because he knows all about Prednisone.
I was not able to get her to accept the med, so I resorted to settling in and just being available for the duration. The total episode duration was probably about 2.25 hours. She had difficulty understanding where she was and why she was here. I imagine that this episode started upon waking, which aligns with Freds' report of the previous incidents. She really wanted all of her stuff here, and has a clutching habit of wanting to hold on to personal items, as if to protect them. I think just being in a foreign environment contributes, but I've seen similar behavior to a lesser scale in the motor home.
In regards to her mental side effects of the steroids - some quick background in case I did not include it before. Mom has had three previous breaks with reality. These are a well documented side effect of this family of medication, and occurs in females more than males. Anti-anxiety medication or anti-psychotic mediation can help with this. One of the problems is that Mom's work in mental health facilities has predisposed her to view anti-psychotic medication as very "heavy duty stuff" that has dangerous effects and side effects.
In her previous episodes, they all occurred after her steroid dosage had been significantly increased (7.5 to 40), with the first episode occurring ~3 days after the increase. Each episode presented as a sudden personality change upon waking from sleep.
This is significant because we are about 36 hours into a massive dosage increase (10 to 120, now at 80). She has had numerous minor verbal slips, such as thinking the dogs are here in the hospital, that wine is in the room somewhere, or that she is in San Diego. These can be midly amusing now, but I'm concerned that they may be indicative of bigger issues over the short-term horizon.
She moved fairly well with assistance. (She has not walked since being admitted.) She consumed some breakfast and a portion of a protein shake. Her O2 was increased to 6Lpm on nasal canula with mild improvement. We were not able to keep her O2 up, so they switched to high volume (full mask with humidifier[?]) at 100% and got her right back to 98% O2. We dropped it down to 40% and lost ground again. After some juggling, they got her to good O2 on the full mask. That lasted for a very short period until she decided that she could not tolerate the mask. She was switched to a more open style mask which seems to be working well.
The doctor came by for a consult/exam. He was initially asking Mom how she was doing today compared to yesterday. She could only reply by asking where Fred was. He tried to engage her again without reply. (She occasionally simply fails to reply to a question or command. If you repeat it several times, she lets you know that she heard you, but is trying to think.)
I had a discussion with him from that point forward. The ultrasound echo from yesterday revealed that her right heart function has significantly decreased since it was last imaged in 2010. He classified this as Right Sided Heart Failure. He stated that this was a result of the pressure in her lungs being higher. The Left side is ~OK with mild diastolic dysfunction. There was pulmonary edema, but nothing that concerned him to a great deal.
He thinks they've probably gotten the max benefit out of the diuretic (Lasix) that they can, and he anticipates backing off soon.
I told the Doctor that we were really looking for a locked-in Diagnosis, Prognosis and Treatment plan. We were also looking to know whether they are attempting to slow her decline, halt the decline, or improve her condition. We would also like to know if this is a chronic condition, terminal disease process or something else. The Doctor said that they are working to provide us with this information. The subtext of his words and body language indicated that we should be braced for no cure for this condition, but without indication of what a timeline or future might look like.
In regards to her need for a Primary Care Physician, he indicated that her current Pulmonologist, Dr. Jon Huseby, could continue to function as her PCP. I had hoped to add an Internist as her PCP to manage her overall care. One option I thought if was to re-engage Dr. Columbo, her previous physician on Camano Island that she had a great relationship with.
In regards to the steroidal psychosis (reality breaks) the Doctor was going to enter an order in to her chart allowing IV anti-anxiety and/or IV anti-psychotic meds in case she suffers a complete break, which I fear is coming.
He did not indicate that a change of room or ward was imminent, which is a change from yesterday. Although the possible move to a general ward I believe was communicated by the nurses.
She was a seen by a Pulmonologist yesterday. They are currently seeing her as a Cryptogenic Organizing Pneumonia case. They are considering additional imaging to help lock down a diagnosis. This may include a CT Scan.
He stated that we should expect to have a consult/exam interaction with him each day. We can relay any questions through staff to have them answered by him.
In regards to an Advanced Directive, I relayed that my personal impression is that Mom's mental state does not enable her to make an informed thoughtful decision on this topic. This would mean that we are left with the default position - they will revive (compress/shock/intubate/vent) if she suffers arrest. From that point forward, all decisions would be made by Fred. He seemed to think that was a reasonable position to be in, but neither he nor I are Mom. I have hunches about what her wishes might be in certain defined situations, but I can't say that I truly know for sure in my heart what she would want.
The Doctor did say that, considering Mom's current condition and the direction she is headed, an Advanced Direction would be needed at some point, but that we are not there yet. This position is not without risks. Should a random failure or event (infection/stroke) happen, we do not have clear direction from Mom on her preferences. Unfortunately, she was not comfortable with the topic when we discussed it in the past, and now that ship has sailed until she has regained mental capacity. This is entirely my personal opinion. I believe that she can probably execute legal documents that would be honored in the case something happened. But I worry that her stated wishes today would not align with her lifelong values, beliefs and desires.
On the down side, I'm sleep deprived, and this may quite possibly the worst presentation of a patient in the history of medicine. I'm sure Rob agrees.
On the plus side, it's great to have Patrick here, and especially to have a fresh set of eyes and ears on things. I also trust him completely to relay an accurate assessment personally to his clan.
Sunday Morning in Seattle
Kim, Fab and I got here about 8:30 this morning. Fred has been relieved and is running out to the motor home to retrieve some objects, and then will get some sleep at our house. We expect to see him later today.I got informed by Fred what happened last night and early this morning. I'm recounting that here, but he can jump in if I got anything wrong.
Mom was administered a form of Haldol yesterday at 3:50pm by IV. She slept from 4-6:30pm, which is the first real sleep she's had. She ate a bunch of soup after that. At 9:15pm she was given her Prednisone, and this was immediately followed by an episode of her speaking gibberish. She also experienced some tremors. When her mental status was checked by the nurses, she was not able to relate her birthdate.
At 11pm, she woke up from sleep nervous and agitated. This occurred again at 2am and was resolved with IV Ativan.
She had a period of lethargy, where verbal interactions resulted in sustained pauses eventually followed by a short grunt or single word.
They tried to reduce her O2 intake to see how she would respond, but did not get good results. A reduction from 4 to 2Lpm resulted in her saturation dropping from 98% to 86%. It still drops on any exertion at all. She is currently back up on 4Lpm.
Looking back, it may have been 4 months or so since we've seen Mom walk independently, and her muscle tone is so reduced that returning that ability seems like a tricky goal.
At 7:30am, she was up, awake and alert. She had an agitated episode, which we arrived to enjoy the end of.
We had a consult with the Doctor this morning. He is Dr. Adam Haugo (Internal Medicine / Hospitalist) with the Polyclinic. He is handling her here in the hospital. We spoke about;
Restoring her personality or using an adjunct therapy to minimize the mental side effects - He thought we were having good results with the Ativan / Haldol. He is going to switch to a prescribed oral medication that is given regularly. I'm concerned that she will not take it (details below), but he thought it was better to prevent episodes than to respond to their occurrence, especially since they cause her O2 levels to drop.
[Mom remains suspicious about her meds. She requires the nurses to thoroughly review anything she has to take, to the point of looking at each pill to verify what it is.]
Current dosing - He has been stepping down on the steroids. She was on 40mg yesterday morning, and 20mg at night. She got 40mg this morning and he'll see how she does today to decide tonights dosage.
We did not see anyone from Pulmonology yesterday. Dr. Lea Smith is reviewing her Pulmonology info and working with Haugo on her final diagnosis, prognosis and treatment. He is hoping that we will hear from her later today.
Haugo is here today and tomorrow, and then off on Tuesday.
He is working to get to the point where her O2 is at a good point, and remains there on exertion/movement.
Kim is going to keep an eye on Finances for Mom and Fred and ensure that their bills get paid.
I'm going to visit with the Financial or Billing office to gauge what the money situation is. I thought they would have been up to talk to us, but that hasn't happened. I'm hopeful that between Medicare and the Supplemental Mom has everything covered.
Mom is currently is a good spot and we are enjoying a nice time with her.
Kerry and Michael Hennessy will be here tonight (staying with us), and John Hennessy will be here tomorrow.
Sunday Evening News
I hope you are finding these updates helpful. It's nice knowing that you are all involved in this situation, even if you may not be here.I should warn you that this update contains news that is really not great. This sentence is a great opportunity to close this message until you are in a supportive setting that is appropriate for receiving bad news. Spoiler Alert: Mom is still alive and fiesty as always.
Mom was able to get a ton of rest today and we credit this to some of the anti-anxiety medicine. She has been groggy but pleasant on waking, although may trend slightly towards agitated about an hour later. But it is nothing like the episodes we were seeing earlier. And one of her sleep sessions lasted about 4.5 hours.
Rob had asked about these meds. I got this info from the Day Nurse, but I missed the timing. I'm pretty sure she's getting Seroquel regularly orally @ 12.5 or 0.125 (it's a pill about the size of a grain of sand.) Mom was told what it was and did not object to it. There are still PRN scripts for Haldol @ 0.5mg and Ativan @ 0.25 or 0.5mg. The nurse related that they've had better results with Haldol.
We finally got to meet with the Pulmonologist who has been reviewing Mom's chart. It was clear throughout the interaction that she had very carefully and thoroughly reviewed Mom's chart completely and fully understood what had been done in the past. She also had consulted with Mom's regular Pulmonologist and received input from him, as well as read all of her test results. This means that we finally received the second opinion that we were hoping for.
They are confident that Mom has smoking related pulmonary disease, which includes pockets of emphysema in each lung. There is Bronchiostasis involvement and Cryptogenic Organizing Pnumonia (COP). But the most important factor may be Pulmonary Fibrosis. This is a permanent scarring of the "engines of the lungs", the Alveoli. These are the very small ends of the lung passages that allow gasses to transfer between the lung into and out of the bloodstream.
This scarring is permanent and non-reversable. In addition, the Fibrosis is a progressive disease, so additional damage is occurring with the passage of time. This means that when Mom inhales, there are not enough alveoli to allow oxygen to enter the bloodstream. And in reverse, there are not enough to allow sufficient CO2 (carbon dioxide) to leave the body. (A buildup of CO2 is what makes you feel like you can't hold your breath anymore.) I'm including a lot of physiology content I learned from scuba, so I'm hoping Rob corrects me if any of this is not correct.
In addition to this lung situation, we also have the heart issues previously discussed. To review, there is right side heart failure and minor diastolic dysfunction in the left heart. They also felt that there was pulmonary edema, and they feel that the diuretic has helped relieve this.
The big picture is that the metric they are looking for so Mom can move out of Intermediate Care is that she can exert herself (Sit up, stand or walk) without her oxygen levels decreasing (desaturating). They always want her O2 to be above 92%. The fact of the matter is that Mom has not had that level of health for at least a year. So we discussed lowering their bar so that Mom could return to some form of her former life. The nurses have discovered that placing Mom on pure O2 @ 40% or higher when she has to move keeps her O2 level right at 100%. The problem is that you can't administer oxygen at that level in a residential setting.
Even more importantly, Mom will continue to worsen as the Fibrosis progresses. As she loses lung capacity, she will deteriorate to the point where they will have to intubate her and place her on a ventilator. We are nearing that point. And the fibrosis rate can become faster with time.
We've accepted that we are headed in a direction that Mom will not be able to recover from. She has a debilitating disease that has run its course for some time and left her very sick. This disease process will result in the loss of her life.
The Pulmonologist related that it is difficult to predict the pace of this process, but she suggested that we may be looking at days, weeks or months. A complicating factor is that Mom's wishes in this regard are not clear. And her mental state is affected by her medication. We are in a gray zone here that we are working to carefully navigate through.
After discussions with the Pulmonologist, we are pursing a course of action where we progressively reduce the steroids that Mom is receiving here in the hospital. This should return her mental capacity. There is a risk that her breathing may worsen, and if it puts her health at risk, we will increase it right back up. But we feel the risk is worth the benefit of having Mom be able to grasp the entirety of this situation. And any health issues could be addressed right here. (Steriods have to be reduced gradually, so it may take a little bit to get off of them, and a bit longer to see if her mental ability returns.)
It's been a while since Mom has had her full mental abilities, so I don't know where her baseline is right now. But even a small window of clarity can help. We would like to get her input on her living preferences and advanced directives.
It sounds like our options include hospice care in a care facility, or home based hospice with staff assistance and support. We are going to engage the hospital social worker and case worker tomorrow to discover exactly what these options are. They explained hospice care in this situation not being a purely palliative approach, but one where they continue therapies intended to mitigate and retard the disease process.
I'll let you know more after we have some meetings tomorrow. I'm going to push for them to happen as soon as possible. The information gathered may result in me having to engage in numerous errands or consultations. So I may not be able to immediately get out a timely update tomorrow.
Due to her short term memory loss (medication related), we have not discussed this prognosis with Mom. We're not trying to protect her from the truth, but rather avoid a situation where she has to learn 5 times a day that we've arrived at the end of this path.
I'm so very sorry that I'm not able to tell you that Mom will be going home and getting better. In the best possible world, we'll be able to get a period of mental alertness where she is able to comprehend fully the situation and it's implications. (At times it sounds like she may be grasping the probable outcome.) We can then clarify her exact wishes, as well as execute any legal documents necessary.
I'm a little tired, but I think the big picture is pretty clear.
Tough Day Today
Sorry for the break in communications. It's been quite the wild ride on this end.First of all, Mom is certainly hanging in there, but it gets tougher by the day. She can have periods where she is really having trouble getting enough air and these are hard on everyone. At times it seems clearer that she has a sense of her condition, at other times; not so much.
There are also periods where she is quite engaged in conversation. But her mental capacity has not been restored with the diminished steroid dosage. We do not believe we will get that back at this point. We are halting the reductions in the steroid dosage.
Away from the daily health monitoring and limited assistance that we can provide, there was much progress on the overall front. My brother Rob arrived last night and got to the hospital this morning. He is an emergency medicine physician and has a wonderful style in interacting with Mom. She trusts him very much and is reassured to have him here.
We had a long and fruitful meeting with the Palliative Care Team. They reiterated that Mom has chronic lung disease. There is no other treatments they can try to fix or halt the progression of this illness. Our focus now is on providing a supportive environment where she can be comfortable. We want to allow her to have a dignified and hopefully painless conclusion to an amazing life, on her own terms.
The palliative team did a great job of guiding us through the difficult process of choosing which medical procedures we would allow them to provide for Mom in the days ahead. First and foremost was the decision that medical interventions such as resuscitation and ventilation are not appropriate for her disease at this point. We have formally executed a Do Not Resucitate order and we will allow Mom to go when she is ready. Our focus has transitioned from monitoring her vital stats to ensuring that she is comfortable. However, we will allow antibiotic treatment of other issues if they arise, but only to provide comfort.
We also had a long discussion about what setting would work best for Mom and the family. We thought we had a good potential candidate facility (Evergreen Hospice) that we were quite hopeful about. And while Hope Springs Eternal, it gets crushed just as quickly in a medical environment. It does not appear that Mom has the coverage required to provide such a facility.
BUT, the social worker who worked with us today was just filling in and had large gaps in her knowledge, despite her best efforts. So we elected to pursue this issue tomorrow with a more knowledgeable expert. And Mom's friend Diana should be here tomorrow, and we hope to utilize her expertise in this field.
We've also had some additional therapies and medications made available that are purely intended to make her comfortable. We're all learning through this process about what that requires, and I hope to get that dialed in quickly.
This update has lots of gaps, as more and more details drop to the floor, inconsequential given the big picture. Every day has it's challenges, and it's bright moments as well. Please let this update afford you an opportunity to reflect on the amazing life my Mom has had, to send good thoughts her way, and to recall a favorite memory of her.
It is better to try than to hope
We are working through this process as best we can, and I wanted to provide you with an update on our current status.So much has happened since my last update that I'm just going to tell you where we are right now. But first, let me tell you that the massive roller coaster nature of a "typical" day is really draining. Every moment of promising news seems to be followed by a crushing setback. At the end of the day, it can feel like your soul has been through a rugby match. But we have awesome support and that enables us to hop right up and charge back in. There is no clear path through all of this, no defined right or wrong. We do the very best that we can, and support one another in a honest and loving manner.
I would like to share a simple example of this roller coaster ride, but it also lets you know our current status. As you may remember from 3rd grade, a hospital is where ailments are treated and illnesses cured. Without a treatable ailment or curable illness, they kinda don't want you in a hospital anymore. So we have had to work with a Care Coordinator, otherwise known as a Health Care Bouncer, to find the best possible place for Mom that meets her needs. In every step of the way up to and including that conversation, Evergreen Hospice has been mentioned as the gold standard facility, and it is close to our house. We spent considerable time discussing home hospice care with the Palliative Care Physicians, but they felt that we would not be able to meet Mom's unique needs in a residential setting.
So we left the care meeting all "gung ho" to move her to Evergreen (hope). But then we learned that Medicare only covers facility services, not the actual room and board. The patient must cover this amount with personal funds, and that runs $250-$350 per day (despair). Then we learned that there are two top notch facilities in Seattle that only require Medicare and the patient doesn't have any out-of-pocket expenses. The Care Coordinator was going to see if she could get Mom into these facilities (hope).
We met with her today (two days after the meeting), and she said that the first facility only accepted Medicaid, and Mom did not meet the criteria (stats and needs) for the second facility (despair). This meant that we were going to have to bring Mom home to my house, and try to keep her alive as best we could (sheer panic). I'm not an expert in health care metrics, but I'm guessing that this would have resulted in a significant reduction in the quality of care. The slightest gap of attention could potentially result in a very threatening event for Mom, and if you've ever let pasta boil over you know how easily that can happen. We asked that the Care Coordinator try the Evergreen facility, just to make sure that they always require patients pay a high cost per day. (We were all in a cold sweat about the terror of having to manage one of these episodes with nothing more than a Hospice support phone number amidst a bevy of barking dogs.)
Fortunately, in the middle of this exchange, Mom's Doctor came by and joined the discussion. She was clearly unhappy about the outcome, and seemed uneasy about sending Mom home with us. She went into an office and privately spoke to the Care Coordinator. Thirteen phone calls, 4 faxes, some counseling for us on how to answer questions, and the big moment arrived. The Care Coordinator came out to inform us that… her shift was over and she was headed home (despair). But she was taking her phone home and would monitor it for a call from Evergreen (feigned hope).
A while later, a nurse came out to tell us….
Evergreen had accepted Mom, with no out-of-pocket money required!!!!!!!!! Hope, real honest to goodness hope. Oh my sweet God, hope and relief and joy and thank you thank you thank you. After an exhausting week, finally some tears of joy. (They taste the same.) Mom will be transferring there sometime Friday.
So, that's where we are right now. We are all quite hopeful, but I'm still guarded. This experience forces you to never let down your guard. We all want to just get Mom into a setting that provides the care that she requires so we can create the perfect environment for her.
On that note, if you have any thought you would like us to share with her, pass those along and I'll print them out for delivery.
I also want you all to know that your expressions of support really help. We all appreciate your kindness and thoughts.
I will let you know how tomorrow goes - stay tuned!
Faith Restored
It is 5pm on a blustery day in the Pacific Northwest. My Mother is laying in a beautiful room at a great Hospice, surrounded by family.There is no need to say anything else in this message. Besides, it's kinda hard to see the keyboard through these tears of joy.

I don't know what to say.
Hi Everybody -I'm writing this update from a mental state where I don't know what to say. But I'm Irish, so I'm going to let my genes take over and I'm sure my finger will find something to type.
The best news is that the Hospice is fantastic! Mom is tended to by a kind care staff, and the family has quickly settled into being comfortable here. There is a hummingbird and other bird feeders right next to Mom's windows, and hummingbirds stop by frequently during the day. We're really striving to provide comfort, dignity and happiness. When waking to this setting, Mom can't believe that she is actually here. It's very clear that this feels like the Presidential Suite to her, and she can't comprehend how a pauper family like ours ended up in the best room in the castle. We tell her to just accept it, but we know in our hearts that a very compassionate act by a caring physician put us here.
We were given the paperwork and requirements to allow dogs into the facility. I called my vet yesterday and they moved heaven and earth to get us in this morning to have Dylan and Sophie examined and get their shots. We took them there and got the approval forms sent to the Hospice. They gave us the approval late this afternoon to have the dogs here. My wife Kim and my cousin Patrick were immediately dispatched to Casa McNichol (otherwise known as Dog Hair Manor) to retrieve said dogs.
Mom has been asleep for most of the day, so she wasn't fully present when the dogs FINALLY entered her room. But Dylan hopped right up on her bed, and Kim and our daughter Kristen were able to move Mom's hands so she could pet the dogs. She hasn't rejoined us yet (and may not ever), but I'm hoping for the briefest moment of being reunited with her beloved dogs.
Dylan did settle in on Mom's bed with her for quite a bit, even resting his head on her leg. I was fortunate enough to get a picture of that moment and have attached it to this message.
I took some time to read out loud the many messages of love and support we've received. I plan to do that again when appropriate. Feel free to keep those coming. In addition, you can leave a message on my phone (425-239-4414) or on my brother Fabio's phone (541-554-8232) and we will play it to Mom so she can hear it. (We may answer the first time you call - just tell us you want to leave a message on the next call.)
You can also send cards, notes, flowers, gifts, or favorite photos to Mom here. The address is;
Evergreen Hospice
Attn: Rosemary Hennessy (Wing 1, Room 3)
12822 124th Lane NE
Kirkland, WA 98034
Unfortunately, I think we may be past the point of phone calls. I'll advise if that changes.
Mom has her eyes closed and we get facial expressions and changes in how hard she grasps hands, so we know she is listening. I've decided to have them halt any medicine that they were giving to suppress her for comfort. I'm hopeful that she has more lucid moments tomorrow, but we might have to resort back to regular medicine if she has problems.
Her husband Fred related that he had some interactions with her today, but I haven't had any since I arrived today. She usually does better in the morning, so we'll see how tomorrow goes.
We are all OK here with Mom letting go and finishing this amazing life. But that does nothing to ease the pain of losing her. She will always be my Mommy and I would give anything to have more time with her, but I do not want that time if she is not healthy. And she is clearly very, very sick. I am bracing for the inevitable impact, but I still won't be ready when it comes. I will never be prepared to wake up in a world where Rosemary Hennessy is not alive. But I will never be without her, as a good part of me is made of her. So I let the pain flow when it comes. Fortunately, laughter and wonderful memories flow just as easily. A strong family and an army of friends stand beside her, even if they may not be here in this room. We feel your good thoughts, prayers and well wishes - and they really, really help. Thank you all for that.
We do not know how much time Mom has left. But we do know that she has made 72 trips around the sun on a giant rock flying through space. And in those trips, measured as years, she has loved, laughed, served, cried, persevered, mothered, comforted, grown and triumphed. We stand vigil in testimony to these moments and her impact on our lives. And we are not waiting for anything, rather soaking up the humbling gift of human life.
I would like to finish this update on a positive note. Think of everything you know about my Mother. Now imagine the most perfect place she could possibly spend her final moments. That is exactly where she is.
Eddie

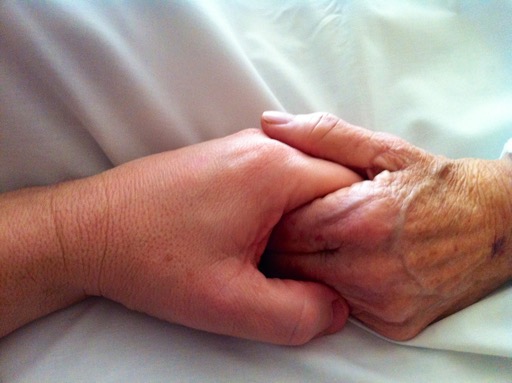
A Life Well Lived
Greetings -On September 10th, 1940, Rosemary Catherine Hennessy came flying into a world that certainly was not prepared for what lay in the future.
In the many years ahead, she would move from a rich white suburb into an inner city ghetto to serve the disadvantaged, hear the whales breach from the beach in Mexico, adopt twin 8 year old boys, live on a plot of land in rugged pioneer fashion, be appointed Superintendent of a state institution for developmentally disabled adults (her biggest accomplishment was shutting down that very same facility), retire, become an EMT, marry and move to magical Orcas Island, travel in a motor home and so much more.
As you know from these updates, she unfortunately became sick, with an illness that took quite some time to drag down a woman of such strong will. And very early this morning, just before 1am, Mom let go of that battle and left us.
My wife and I, my brother and cousin were present, as were both of Mom's dogs. It was calm and peaceful, and we were all relieved that the fight was over. Her day was spent in a sleep state, but her ears were still clearly listening. She had visits from friends and family. Later in the day, her loving husband Fred said his peace with her and made it clear to her that he was leaving for the night.
The nurses noticed a sharp drop in her condition shortly after that. They were surprised at the speed of the decline. (There were no medications involved.) My brother Fabio had an opportunity to speak to her, and he left to run a quick errand. I spent about 20 minutes speaking to her.
I let my Mom know that she had lived a rich life, with many people who loved her very much. And I let her know that we had all received everything we needed from her, and that we were all going to take care of one another. I kept telling her that we are all ok. That we are family, and we will take care of one another.
This has been a difficult week. And now that this episode is over, I am left with a sense of peace. The medical struggles have evaporated, and revealed a lifetime of warm memories and funny stories. We all feel very good about the efforts we made here. And we are relieved that this long struggle is over.
There are more things about my Mom that I'll miss than I could ever list here. Mom's final wishes will be followed, and my daughter Kristen is handling this for the family. I will update you all as soon as we have information.
I think that your messages of support, which were read to Mom this afternoon, brought her comfort in her final moments. I thank you all for the amazing support that has carried us through such trying times.
As a young boy, I told my Mom that I would one day change my name to Eddie Hennessy. She told me that wasn't necessary at all. I know now that I have all the Hennessy I'll ever need in my heart. And I think she knew that even back then.
Goosebumps and Chills
Daybreak yesterday found us surviving in a strange new world without Mom. We woke far too early to meet at the cemetery and select her final resting place, especially considering the breakfast we had of beer, irish whiskey and cake when we finally returned to the house from hospice. I wanted to take a moment to relay what seemed like an inconsequential detail of the events Saturday night.After I had a chance to talk to Mom and release her from anything she worried about here, Kim and I sat with her in silence, so as to not disturb the process. A while into that quiet period, my daughter Kristen sent me a text message asking me to play a certain song in the room. (She had wisely chosen not to remember Mom as a dying woman, and elected to stay home.) Playing music seemed like it would disturb the mood, but I felt it would be wrong not to honor Kristens' wish. I pulled my chair close to the hospital bed, turned the volume up on my computer, and called my daughter.
When she answered, I simply said, "Listen to this". I then played the song and allowed Kristen to listen. Twice during the song I observed a very noticeable change in Mom's facial expression. At the end of the song, I very quietly asked Kristen if she wanted to say something to her Nana. Through her sobs, I could make out "No" and she hung up. Forty five minutes later, Mom was gone.
Sunday morning, Kristen told me that when she was out visiting Mom at Thanksgiving, she had some private moments with her. Mom worked with Kristen on her final wishes (which Kristen is currently executing perfectly). And they reminisced about their times together, including attending Riverdance - the Irish dance performances. Mom had discussed that very song to Kristen, as Mom used to sing it to her. Mom said that if she was ever one of those people that is sick in bed and is not letting go, Kristen was to play that song so Mom will know that it was time go.
Life, and death, are amazing.